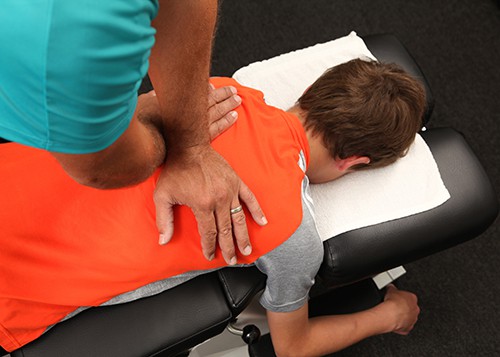
Chronic low back pain can have a huge impact on a person’s quality of life. According to a recent study, the lifetime prevalence of low back pain in the United States may be as high as 84%.[1] The prevalence of chronic low back pain is about 23% and it disables 11 – 12% of the population.[2] Treatment options are available over a wide spectrum, and many people resort to over-the-counter medications or prescription opiates to control this pain. As we know, these opiates have their own set of risks and can be highly addictive.
In a recent comprehensive review, a group of researchers looked at a large number of studies that have been done on low back pain from 2000 to 2017. They determined that there was moderate quality evidence that spinal manipulation produced up to a moderate reduction in pain intensity compared to just exercise and physical therapy.[3] Thrust-type treatments were also likely to reduce disability for patients compared with other active treatments.
The researchers in this 17-year review studied 51 trials (from 711 articles reviewed). There were 8,748 participants across the 51 trials.[4]
Some key points from the study review include:
- Mobilization and manipulation therapies are widely used to benefit patients with chronic low back pain.
- In treating low back pain, “many physicians rely on non-steroidal anti-inflammatory drugs, opioid, and neurotropic medications, or steroid injections and surgery as their main tools. Because of the potential or apparent risks associated with these tools, non-pharmacological approaches, thought to involve minimal adverse events, have become popular.”
- Recent systematic reviews suggest that spinal manipulation and mobilization are ‘viable’ options for pain treatment.
- Spinal manipulation is defined as “the application of high-velocity, low amplitude manual thrusts to the spinal joints slightly beyond the passive range of joint motion.”
- Duration of low back pain:
- In 60% of included studies, the average pain duration was of 3 months or more.
- In 12% of included studies, the average pain duration was of 6 months or more.
- In 28% of included studies, the average pain duration was more than 1 year
- The majority of studies involved physical therapists, chiropractors, physicians, naturopathic, or osteopathic clinicians.
- Mobilization and manipulation treatments were largely safe.
Conclusions from the review:
- There is good evidence that manipulation (i.e., thrust) treatments may produce up to a moderate reduction in pain compared with other active treatment options alone, such as exercise.
- Thrust interventions are also likely to reduce disability for patients compared with other active comparable interventions.
- The beneficial effect seems to increase over time at 3 and 6 months follow-up. There is some evidence that mobilization (i.e., non-thrust) treatments alone may have a diminished effect compared with other active treatments in terms of reducing pain intensity or disability.
- Programs that blend multiple types of treatment may be promising options. More research is needed to assess other important patient outcomes in order to strengthen the evidence between mobilization and manipulation for reducing disability, and increasing the health-related quality of life for patients with chronic low back pain.
- The research to date is still varied, and questions remain about optimal treatment duration, dose requirements, practitioners to be involved, and the kinds of patients who may benefit the most.
This review confirms what we already knew; namely, that manual therapy can be a safe and effective treatment strategy for those suffering from low back pain, whatever the cause. As our clients are at the center of everything we do, we remain committed to keeping our readers informed of interesting and informative medical studies such as this one.
[1] Manipulation and mobilization for treating chronic low back pain: a systematic review and meta-analysis. Coulter et al.; The Spine Journal 18 (2018) 866-879.
[2] Ibid.
[3] Ibid.
[4] Ibid.
